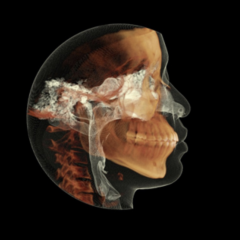
The Department of Oral and Maxillofacial Medicine and Diagnostic Sciences has received accreditation of its Cone Beam Computed Tomography (CBCT) scans through RadSite—making the school the first in Ohio to receive this accreditation.
Overseen by Associate Professor Ali Syed, the program's successful accreditation directly translates to improved patient outcomes and healthcare quality and instills confidence in a higher standard of care.
The 2023 Homecoming and Reunion Weekend was held Oct. 12-14. Alumni enjoyed many events including a Welcome Reception at the House of Blues and a live Yomi Robot surgical demonstration.

In anticipation of the upcoming Class of 2024 Commencement Ceremony, we are showcasing several graduating students over the next couple months!
Rowan Chinwalla's favorite memory is attending the Dental School formal and getting to enjoy a great night with friends, classmates and faculty.




